
The frequency of patients seeking access to telehealth services has risen dramatically since the pandemic in 2020. Consequently, there has been a consistent increase in the development of two-way telecommunications technologies to enable better Remote Patient Monitoring (RPM) and care delivery.
Several HealthTech companies have been pioneering the integration of Artificial Intelligence (AI), cloud computing, and data analytics to further advance the quality of telehealth software development. The Centers for Disease Control (CDC) and Prevention observed that there had been a 50% increase in telehealth visits in 2020 from the previous year.
Along with recent trends in technology adoption among civilians, the CDC report is evidence that the demand for remote patient monitoring software is unlikely to die down any time soon. In this article, we will attempt to create a definitive guide that can equip you with the necessary high-level understanding for the development of efficient remote patient monitoring systems and applications.
Integration Tips for Remote Patient Monitoring Systems
The US Department of Health and Human Services (HHS), the federal government's branch promoting the improvement of citizen health, defines certain parameters for the implementation of remote patient monitoring. As the RPM practice gains prominence in the telehealth domain, here are the HHS' tips for its implementation in your healthcare practice:
Care Delivery and Management
When starting out with RPM adoption, you must ascertain which areas of your care delivery and management are to be improved upon. With an RPM system built into your legacy systems, a number of acute and chronic conditions can be monitored and managed including but not exclusive to the following:
- High blood pressure and cardiac conditions: Remote blood pressure monitoring cuffs can read and send relevant and timely data to your Electronic Health Records (EHR) for ad-hoc and post-monitoring review.
- Diabetes: You can track patient blood sugar levels with glucose monitors connected to the cloud.
- Weight management: Smart scales equipped with Bluetooth can be paired with wearable fitness trackers and are quite popular among fitness enthusiasts.
- Chronic Obstructive Pulmonary Disease (COPD): COPD is a condition wherein airflow to the lungs gets obstructed, which can be monitored using photoplethysmography and respiratory force sensors.
Tips for Implementation
When planning to integrate RPM into your existing systems, you must chart a step-by-step implementation blueprint that takes into account the following elements:
- Patient Education: An effective RPM implementation program must also include the training of patients to use the system over the patient-facing mobile or desktop application. They must be trained around the module for usage during doctor appointments in addition to written SOPs in place. Patients must be made aware of how their vitals will be recorded and shared across the RPM system. Moreover, they should be encouraged to ask questions at every turn or email the questions later.
- Billing and Reimbursement: Patients need to be educated about the precise coding and billing language they should fill in where Medicare claims have coverage for RPM. HHS says that the precise term to be filled for this purpose is "remote physiologic monitoring".
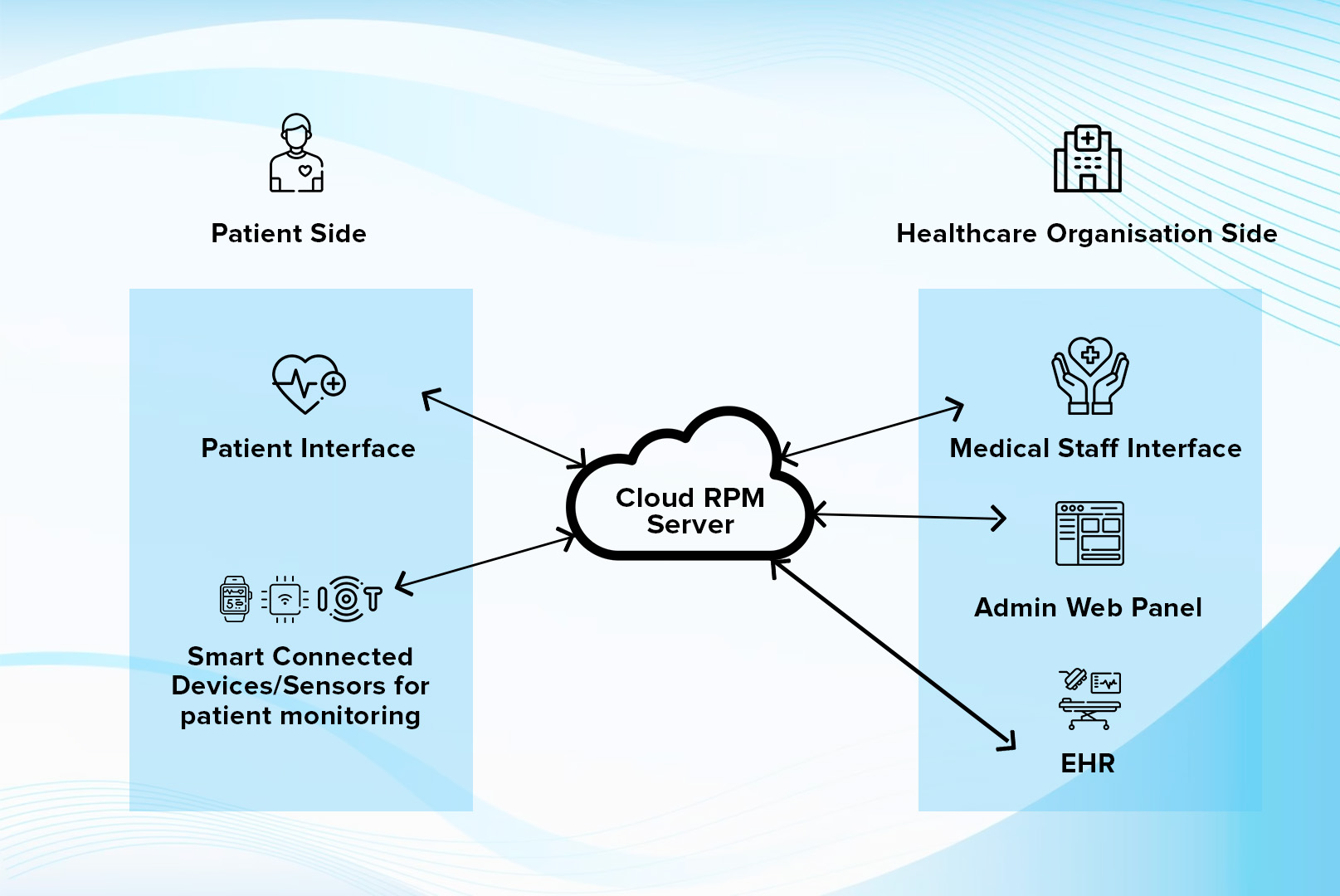
Steps to Build Reliable RPM Software
Healthcare Software-as-a-Service (SaaS) providers need to spend enough time gathering first-person insights about users' needs. This is the only way to build an RPM system that ensures complete patient satisfaction. Here are the steps involved in developing an efficient RPM software system:
1) Requirements Gathering
The requirements-gathering stage consists of the following steps:
- We need to define the stakeholders, i.e., who all are going to be using and impacted by the system such as healthcare providers, patients, caregivers, and administrators.
- Conduct a needs assessment wherein you review current patient monitoring practices, identify areas for improvement, and evaluate the resources needed in terms of infrastructure setup, system requirements, technology stack, etc.
- Next, you must define the functional requirements such as what the vital signs of the patient must be monitored, and non-functional requirements such as the performance metrics of the system in terms of response time and accuracy.
- You need to prioritize and validate the requirements by conducting patient surveys and focus groups.
2) System Architecture Design
Designing the system architecture of the RPM system involves continuous communication with the relevant stakeholders to understand the overall scope and impact of the final system design. Here are the steps to implement the same:
- Consult with medical professionals, patients, and IT specialists serving as admins to understand the actual scope and requirements of the system.
- Define the sources of patient data such as sensors recording vital signs using wearables and other devices, previous health records, diagnostic history, etc.
- Choose the most viable mode for communication and a database that ensures the utmost security and data privacy.
- Design an easy-to-use interface that physicians and patients can both learn to use quickly.
- Ensure that the system architecture is scalable, constantly test and validate it and conduct continuous monitoring for reinforcing its security and reliability.
3)Develop Software and Ensure Hardware Integration
The implementation or development stage of the RPM system involves the lion's share of the overall software development lifecycle. The different sub-stages that are part of the development include the following:
-Setting Up Modules: Each module of the remote patient monitoring system is self-contained and carries out a specific function. These modules should be well-organized along with ensuring that the code is extensible, scalable, and can be maintained robustly. These are some of those essential modules:
- Clinical Dashboard: All the patient health alerts, notifications, and communication with the patient is carried out here. Patient data can be viewed and managed with ease.
- Patient Application: Patients can leverage this module to record and input their vitals via wearables and other sensors. Other features of the module are appointment scheduling, medication reminders, and communication with medical professionals.
- Data Analytics: Patient data analytics provide insights into the patient's ongoing condition and diagnostic history for holistic decision-making. Machine learning algorithms can be integrated here for predictive health outcomes and anomaly detection.
- EHR Integration: This module connects the RPM system and patient data with the Electronic Health Records (EHR) for setting up all-around context about the patient.
- Wearable Device Integration: Fitness trackers and smartwatches are integrated into the system for the automated upload of patient data into the RPM workflow.
-Programming the RPM: After choosing the most viable technology stack in terms of the programming languages, databases, and frameworks, the actual writing of the code takes place. Following the most advanced coding standards, write properly annotated lines of code that are secure and scalable.
-UI Development: The User Interface (UI) for the system should be developed with the aim to make it seamlessly responsive and platform-agnostic.
-Database Development: The database should be developed keeping it aligned with the healthcare industry's most essential standards of compliance such as Physician Self-Referral Prohibition law and Civil Monetary Penalty law. Additionally, HIPAA compliance must also be kept in check for ensuring the protection of sensitive patient data.
-Version Control: An efficient version control system must be set up to track code changes and ensure codebase consistency, as the development team follows best practices for branching and merging the codebase.
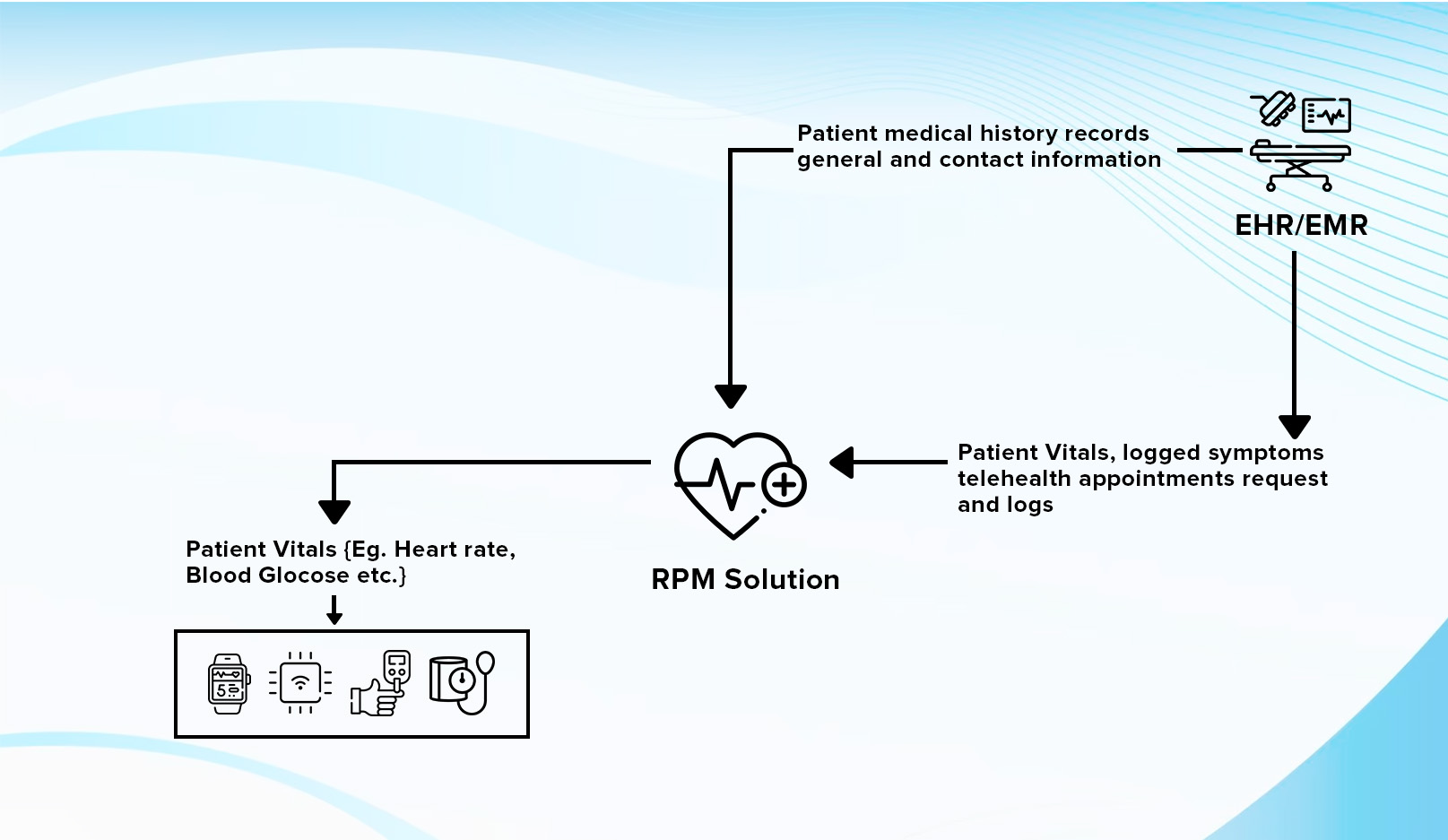
4)Test and Validate
The testing and validation of the RPM system are essential since there is a need to ensure that the system meets the relevant requirements. Here are the steps to be followed for the same:
- Develop an exhaustive test plan for testing all elements of the system including ensuring that the functional requirements, user experience, security features, and performance are all up to the mark.
- Carry out unit testing for each component, integration testing for all modules, and system testing.
- Take the system through various conditions of user overload and other situations to keep it prepared for load and unexpected stress.
- Test the relevance, accuracy, and validity of the data that is fed to the system and generated by it.
- Also, test the ease of integration and communication with other systems such as EHR and wearable devices and sensors.
5) Deploy the RPM System
The deployment of the system to its stakeholders should only be carried out after all the pre-requisite steps for deployment have been accounted for. Here are the steps involved in the deployment of the RPM system:
- Determine the final system infrastructure in terms of the hardware, software, and network components of the overall RPM system.
- Define all the elements of the deployment plan including the scope of the system, resources needed, deployment timeline, and stakeholders impacted.
- Ensure that the healthcare providers and patients have been trained well on how to use the RPM system properly in the production environment.
- The system should work well with wearable devices, external systems, and sensors in the production environment.
- Roll out an initial version, possibly a beta, to a select group of healthcare providers and patients, to gauge whether the system works well before deployment. Based on the degree of success of the beta, the final version can be rolled out gradually.
- Evaluate the impact of the system on patient outcomes and the healthcare delivery workflow and see if the intended impact was attained.
- Continuously survey the stakeholders and test the system to meet the evolving needs of the providers and patients.
ALSO READ: Remote Patient Monitoring Systems: Major Components, Relevance and Types
Elevate Care Delivery with RPM Systems
With advancements in technology, it is becoming easier and more cost-effective to create such systems. However, it is crucial to carefully consider the needs of patients and healthcare providers when designing and implementing the system. By following the guidelines outlined in this guide, you can create a remote patient monitoring system that benefits both patients and healthcare providers. To learn how you can build a system that is user-friendly, secure, and able to provide accurate information to healthcare professionals, you can book a free consultation with Daffodil Software today.



